Where your smile makes our day
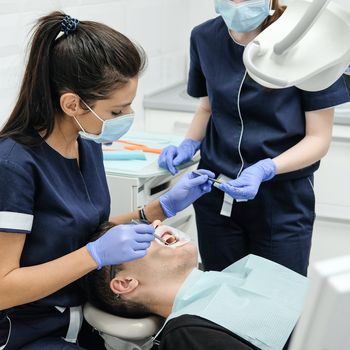
Welcome to our lovely dental practice! We are pleased to offer truly comprehensive dental care in Port Charlotte, Florida. Our skilled and knowledgeable team have worked together for many years to provide you with the best possible care. We strive to care for you in a comfortable and caring environment where Dr. Tony Menendez anticipates your needs and communicates your dental treatment options clearly. Our team is bilingual, speaking both English and Spanish, and, as an added bonus, our therapy “pup” is known to calm even the most anxious patient. We believe in striving to be exceptional in all our care and are glad to have it define us:
Ex-cep-tion-al Den-tis-try (noun): exemplifying a dedication to compassion, artistry, comfort, technology, experience and education.
We invite you to contact us today at 941-624-4575 if you would like to learn more about our services or if you would like to schedule an appointment with our accomplished dentist.
Read More
Our Top Services
Comprehensive Dentistry
Comprehensive dentistry is a holistic approach to dental care that focuses on treating the entirety of your oral health needs...
Read MoreRestorative Dentistry
Restorative dentistry is a specialized field that aims to repair and restore damaged or missing teeth. It goes beyond just fixing the appearance of your smile...
Read MoreAesthetic dentistry
Aesthetic dentistry is a branch of dentistry that focuses on improving the overall aesthetics of your smile.
Read MoreImplant Dentistry
Implant dentistry is a type of restorative dentistry that replaces missing teeth with artificial tooth roots or implants. The implants are …
Read MoreWhy Choose Us?

PASSION FOR SERVICE
Our dentist and team love what we do and enjoy working one-on-one with our amazing patients every day!

OUR AMAZING TEAM
All of our team members are highly skilled, experienced and up to date in the ever-changing dental field.

STUNNING RESULTS
We are committed to giving you an impressive and beautiful smile you can be excited to share with others!
Meet The Team

Dr. Tony Menendez
Dr. Tony Menendez opened his dental practice in Port Charlotte, Florida, in 1986. He is a graduate of Emory College and Emory University College of Dentistry in Atlanta, Georgia. He is dedicated to the philosophy of the Academy of General Dentistry and the pursuit of lifelong learning. He is a graduate of the two-year Comprehensive Dental Program of the University of Florida College of Dentistry. Dr. Menendez was awarded a fellowship in the Academy of General Dentistry (FAGD) after passing a rigorous exam and completing over 500 hours of continuing education in 2004. Upon graduation from the Comprehensive Dental Program, Dr. Menendez continued as a visiting faculty member at the University of Florida College of Dentistry, working with Comprehensive Dental Program participants. He is pleased to use his expertise to provide dental care in Port Charlotte, Florida, and help you achieve a brilliant smile! ¡Se habla Español!
info

8

7

6

5

4

3

2

1
Gallery
Office Hours
MON - THU8:00 am - 5:00 pm
FRIBy appointments only
SAT - SUNClosed
TONY MENENDEZ, DDS, MAGD
Location
4120 Tamiami Trail Suite A,
Port Charlotte, FL
Phone : (941) 624-4575Text Us : (941) 624-4575